Many Canadians are unaware of their risk factors for glaucoma
By Cynthia N. Lank
As we take in the world around us in all its colour, shapes, contours and beauty, the simple act of seeing, which so many of us take for granted, is actually incredibly complex. The human eye is a marvel of evolution, design and engineering. Our eyes capture light, which is sent via the optic nerve to the brain, where it is converted into the images we see. Just like blood pressure in our body, the eye needs to maintain a healthy level of pressure—not too high, not too low. If the internal pressure in the eye (known as intraocular pressure or IOP) is too high over time, the optic nerve can become damaged and its ability to transmit signals to the brain can become impaired.
The result is glaucoma, which if untreated in its early stages can lead to vision loss. Glaucoma is a chronic disease, for which there is no cure. Once a person is diagnosed with glaucoma, reducing the pressure in their eye(s) is the only way to protect them from continuing to lose their vision. Ophthalmologists do this with medications (eye drops and sometimes oral medications), laser treatments or surgery.
Winchell, a 46-year-old Montrealer working in the aeronautics industry, describes his diagnosis of glaucoma as totally shocking, as he had absolutely no symptoms. Winchell was in the market for a new pair of prescription sunglasses, which his health insurance would cover only after an eye exam. But his visit to the optometrist, for what he thought would be a simple vision check, turned into a journey to try to save his vision. When his optometrist detected high IOP in both Winchell’s eyes, but especially his right eye, she referred him to Dr. Hady Saheb, an ophthalmologist and glaucoma specialist at McGill University Health Centre.
Dr. Saheb immediately started Winchell on a regimen of daily eye drops to lower his IOP. However, after several months of follow-up, his IOP was still elevated and unstable. The next steps included two different laser treatments and, finally, surgery. Winchell’s regimen of daily eye drops and frequent follow-up to monitor both eyes will continue for the rest of his life. He describes the stress not only of his diagnosis, but also of the reality of living with a chronic disease, “The weird thing is that you don’t feel anything, you feel good, and you don’t have any eye changes, but the pressure is not working properly, and then boom! You can lose your vision. Now I am living with something permanent and ongoing for the rest of my life. Every time I go back for a follow-up I am scared, I am just keeping my fingers crossed, I don’t know what to expect, because I don’t feel anything different. This is still shocking for me.”
While his diagnosis came out of nowhere, Winchell has since discovered that he was in fact at high risk for glaucoma, with his age (over 40), his African heritage and a family history (he learned his paternal grandfather had glaucoma) all increasing his risk. Millions of Canadians share these very risk factors, yet they may not appreciate the silent nature of glaucoma and the fact that once vision is lost, it cannot be restored.
[Pull quote] The Canadian Ophthalmological Society reminds all Canadians that, in its earliest stages, glaucoma has no noticeable signs or symptoms. For this reason, it is it difficult to diagnose without regular eye exams that include specific testing for glaucoma. Be sure to tell your optometrist if you have a family history of glaucoma. Monitoring over time is needed to detect changes in the pressure in the eyes and changes in the visual field. As glaucoma progresses, peripheral (side) vision loss occurs and sometimes even central vision loss can occur. If left untreated, it will progress to tunnel vision, then blindness. Once vision loss occurs, there is no way to reverse it.
Glaucoma is the second-leading cause of blindness in the world. More than 400,000 Canadians have glaucoma and many more in our aging population are at risk for developing glaucoma and other age-related eye diseases such as cataracts, macular degeneration and diabetic retinopathy. The good news: Regular eye exams can detect these diseases in their earliest stages so that treatment to slow their progress can begin. Winchell’s advice: “Don’t be too complacent. It is really very important to know your risk factors for glaucoma and have regular eye exams. Glaucoma can really affect you and threaten your vision.”
The gift of sight is so precious—maybe today is the day to make that appointment with your eye doctor.
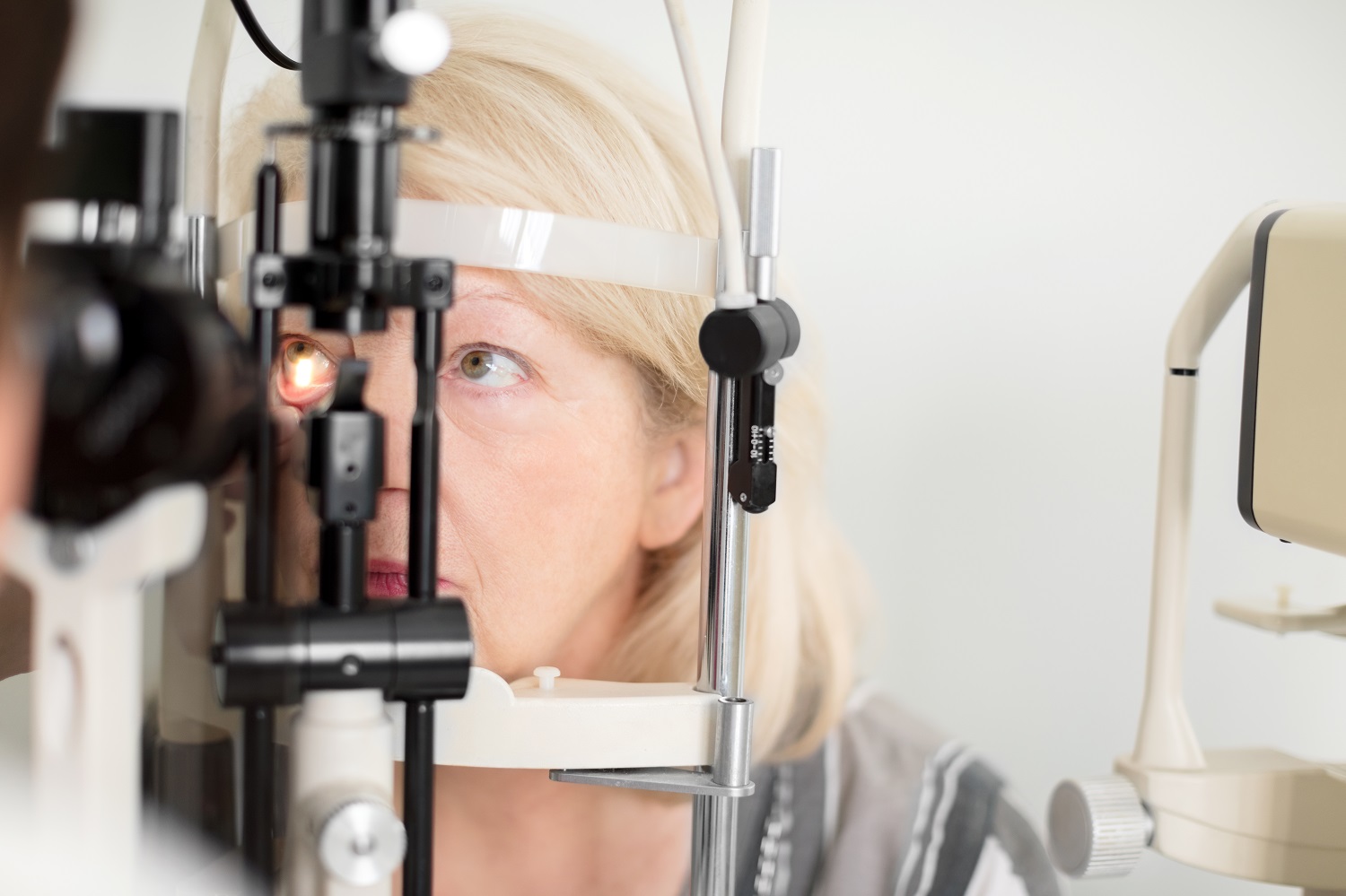
Caption for image:
Tonometry is one of several methods used to screen for glaucoma. This test measures intraocular pressure by recording how the cornea (the clear outer layer that covers the front of the eye) responds to the touch of an instrument or a quick puff of air. There is no pain or discomfort, as the eye is first numbed with drops.
[Sidebar]
Glaucoma Risk Factors
Find out if you’re at risk for any of “The Big 5” eye diseases (cataracts, glaucoma, diabetic retinopathy, age-related macular degeneration, and eye injury) by taking the assessment at this link: https://www.seethepossibilities.ca/eye-health/risk-assessment/ |
Cynthia Lank is a freelance medical writer in Halifax, Nova Scotia. She has written extensively on eye health topics and was the executive editor of six ophthalmology clinical practice guidelines.
| For more information about glaucoma …
Canadian Ophthalmological Society · Ask the Expert: Dr. Hady Saheb answers common questions about glaucoma https://www.seethepossibilities.ca/ask-me-anything/ · Patient information: Downloadable pamphlets on glaucoma (and other common eye diseases) in English, French, Arabic, Chinese and Punjabi. Visit https://www.seethepossibilities.ca/eye-health/glaucoma/ Canadian Glaucoma Society · Patient information on glaucoma with detailed information on testing and treatments. Visit https://cgs-scg.org/information-about-glaucoma/ |
This article is not intended to provide individual medical advice or replace the advice of an eye care professional.






